Podiatrists: Occupational Risks Related to Indoor Air Quality and Prevention Strategies
In summary
- The profession of podiatrist is among those most exposed to indoor air pollution: PM2.5 fine particles from drilling and sanding, volatile organic compounds (VOCs) emitted by adhesives, solvents, and disinfectants, and biological aerosols.
- Repeated exposure may be linked to chronic respiratory problems, nasal polyps, occupational asthma, allergies, headaches, or eye irritation.
- Without actual measurements, these exposures remain invisible: two rooms that look similar may have very different levels of pollution.
- The recommended approach consists of three steps: first, measure; then, address the sources; and finally, treat any remaining pollutants.
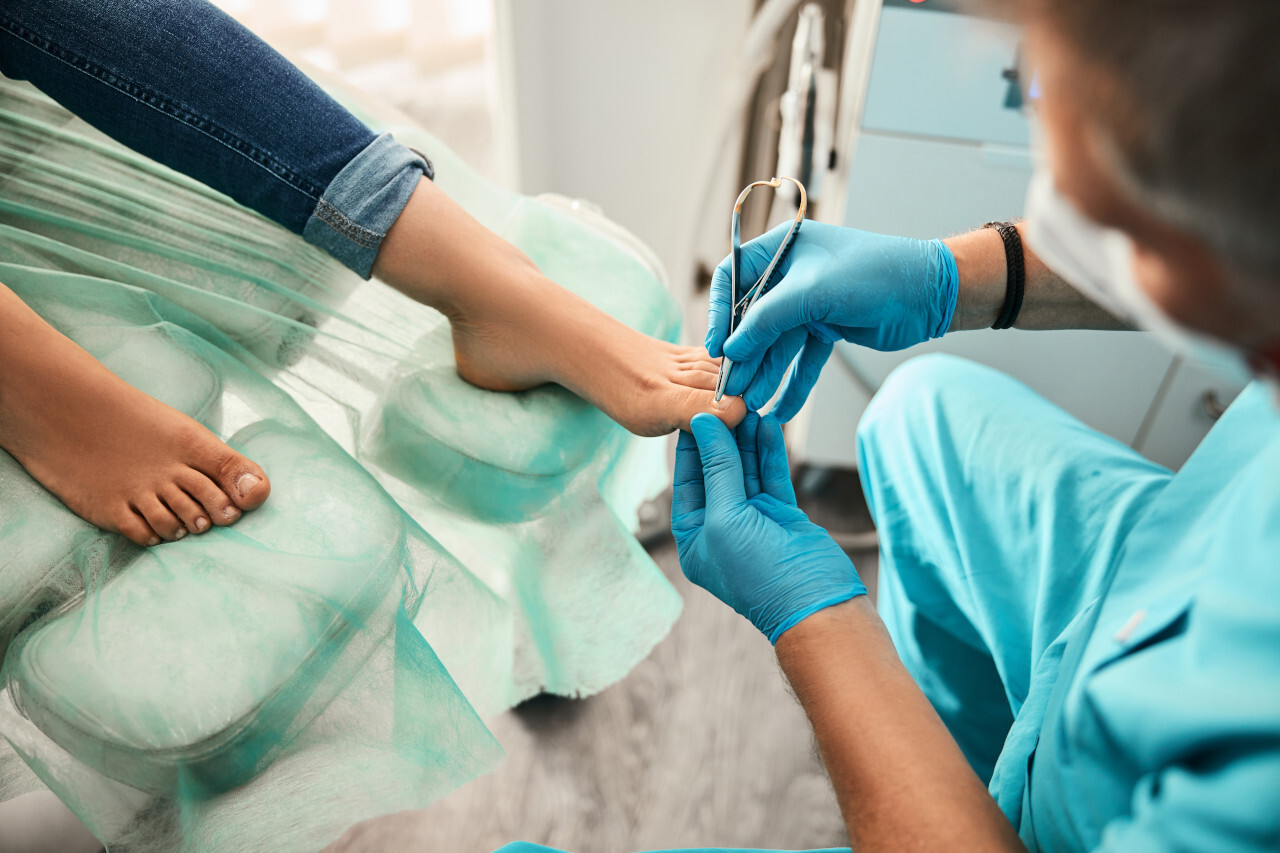
Every day, podiatrists are exposed to drilling dust, volatile organic compounds (VOCs), biological aerosols, and various chemical agents generated by their work. Yet in many practices, these pollutants remain unseen and are rarely measured. Indoor air quality is now a significant occupational health concern for exposed professionals.
Long underestimated, these occupational risks related to air quality in podiatry practices are now part of a more comprehensive approach to prevention, workplace comfort, and collective protection. NatéoSanté podiatrists in this effort, in partnership with the National Federation of Podiatrists (FNP).
Why are podiatry practices particularly at risk?
The work environment of a podiatrist involves several sources of pollution that reinforce one another:
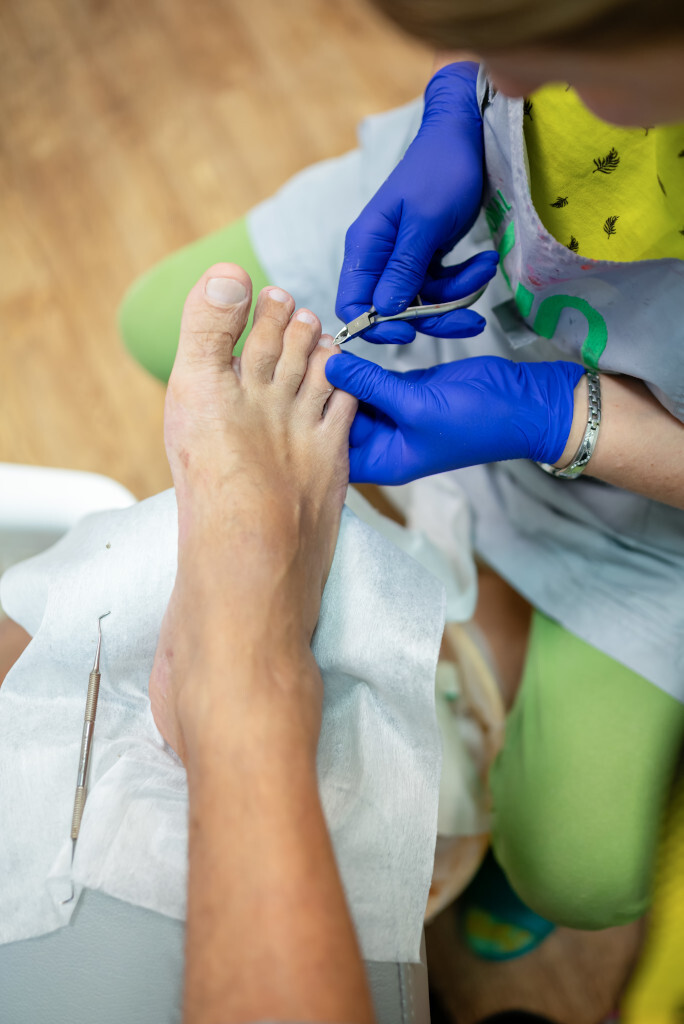
- Technical procedures that generate dust: trimming thickened nails, sanding calluses, and cutting and shaping orthopedic insoles
- Everyday chemicals: neoprene adhesives, solvents, surface disinfectants, resins, cleaning products
- Often older buildings: over the years, walls, floors, and furnishings gradually absorb VOCs, creating a persistent source of background pollution even when the products are not actively in use
What pollutants are found in a podiatry office?
Fine particles and milling dust
Milling and sanding operations generate a significant amount of fine particles. The smallest particles, particularly PM2.5 and PM1, can remain suspended in the air for long periods and penetrate deep into the respiratory tract. Even when equipment is equipped with extraction systems, some of the particles continue to spread throughout the office.
These particles may contain:
- keratin fragments;
- fungal agents;
- bacteria;
- resin dust or synthetic material dust.
“As podiatrists, we are highly exposed to pollutants: fine particles and dust generated during sanding, during treatments, and when shaping orthopedic insoles.” Candice Plana, podiatrist, Talence (33)
VOCs: Persistent Chemical Pollutants
Volatile organic compounds (VOCs) are a group of chemical substances emitted in gaseous form by adhesives, resins, solvents, disinfectants, and certain coatings.
Some products used in the workplace may contain substances classified as carcinogenic, mutagenic, or toxic to reproduction (CMR). Others may cause mucosal irritation, headaches, or allergic sensitization over the medium term.
In older offices, these compounds gradually seep into the materials over the years, creating a source of background pollution that is difficult to eliminate without thorough cleaning.
“My father, who used to work at the practice, had developed nasal polyps from breathing in indoor air pollutants over many years.” Candice Plana
Among these chemical sources, biocidal products—such as disinfectants, sprays, wipes, and surface sanitizers—are often underestimated because they are perceived as hygiene products rather than sources of VOCs. Changes to the regulatory framework surrounding the Certibiocide certification program underscore the importance of product selection, storage, and ventilation during use.
Biological aerosols
Nail filing and certain procedures produce aerosols that may contain fungal or bacterial agents. These biological aerosols pose a particular challenge in healthcare professions and public-facing environments.
Health effects: what the literature says
A cross-sectional study of 1,353 French podiatrists (ONPP/University of Rouen, 2021) found that risks associated with dust and chemicals are among the primary occupational hazards in the profession.
The most commonly reported side effects are:
- respiratory disorders: chronic rhinitis, asthma, nasal polyps
- eye and upper respiratory tract irritation
- recurrent headaches associated with exposure to solvents
- skin sensitization and allergic reactions
These symptoms often develop gradually, making it difficult to identify a link to the workplace.
Odors and discomfort: the first warning signs
Persistent odors, a stuffy feeling, irritation, or headaches at the end of the day are often the first signs of a buildup of pollutants.
In many dental offices, practitioners eventually stop noticing certain odors—a well-documented phenomenon known as sensory habituation—while patients still perceive them quite strongly.
“I was getting a lot of complaints from my patients about odors that bothered them—odors that I myself could no longer detect, except when I was in the gluing area of my workshop.” Candice Plana
Persistent odors in a room are often an indirect indicator of poor indoor air quality and warrant an objective measurement of the pollutants present.
Risks that are difficult to assess without measurement
Without measurements taken under real-world conditions, it is often impossible to accurately identify the main sources of pollution, exposure peaks, or the actual effectiveness of the measures implemented.
Pollution levels can vary significantly depending on:
- the number of patients and the care provided;
- methods for manufacturing orthoses;
- the products used;
- ventilation of the room;
- the layout of the rooms.
Two offices that look similar may therefore have very different levels of pollution.
Tests conducted in podiatry clinics consistently show significant fluctuations throughout the day: peaks in fine particulate matter and VOCs occur during drilling, when chemicals are used, or when air exchange is insufficient.
“In my office, it took about nine months for the VOC and PM2.5 particle sensors to drop to their lowest levels, which clearly shows just how deeply the pollutants had permeated the space.” Candice Plana
Air Quality and Occupational Risk Prevention
Indoor air quality is an integral part of occupational health and safety and workplace risk prevention.
Exposure to dust, aerosols, and chemicals found in dental offices can prompt reflection on:
- occupational risk assessment;
- collective prevention;
- the layout of workstations;
- air exchange;
- and the selection of appropriate equipment.
In this context, exposure to dust, chemicals, or aerosols in dental offices may prompt further consideration of the Single Document for the Assessment of Occupational Risks (DUERP).
Measuring air quality thus makes it possible to objectively assess certain exposure situations and implement measures that are appropriate and proportionate to the practice’s actual activities.
How can you assess and improve the air quality in your office?
Step 1 – Measure: Make the Invisible Visible
Before making any equipment-related decisions, an indoor air quality audit conducted under normal operating conditions allows for:
- to objectively measure VOC and PM2.5 levels;
- to identify peaks associated with certain activities;
- to assess the effectiveness of air exchange;
- to prioritize corrective actions.
NatéoSanté diagnostic services conducted directly in doctors’ offices, using monitoring devices that track changes in pollutant levels over several days.
Step 2 – Addressing the root causes: primary prevention
Primary prevention remains a priority: choosing products with lower emissions whenever possible, working in a well-ventilated area when applying adhesives, limiting cumulative exposure, adapting the layout of the workspace…
For example, grouping activities that generate the most dust—such as the sole-making workshop—in a separate area from the treatment room can help reduce certain exposures.
Step 3 – Treat residual pollutants
For residual pollutants, particularly in high-volume medical practices or older facilities, additional air treatment solutions may be considered based on the results of the assessment.
- HEPA filter for fine particles (PM2.5, sanding and milling dust)
- High-density activated carbon filter for VOCs, adhesives, solvents, and odors
- High-efficiency filtration and complementary technologies for biological aerosols (fungal and bacterial agents)
The design must take into account the volume of the room and distinguish between the treatment room and the insole production area, which have very different levels of contamination.
Podiatrists work in a professional environment that is more polluted than it appears. Chronic exposure to fine particulate matter, VOCs, and biological aerosols—which is often invisible and gradual—can have a lasting impact on practitioners’ working conditions.
Making the invisible visible is the first step in an effective approach: measuring and understanding the sources of pollution, and then implementing measures tailored to the practice’s actual operations.
Sources: ONPP (2021 Occupational Risks Report, 2024–2025 Updates), University of Rouen Normandy (DUMAS Thesis, 2022), Idélia Santé (Certibiocide, 2025), European Regulation (EU) No. 528/2012, Certibiocide Order, September 2025, INRS.